Despite Decades of Increased Spending, the Veteran Suicide Rate Continues to Rise
Veteran suicide remains a national crisis. Despite decades of effort and billions of dollars spent, the numbers haven’t meaningfully improved. In some areas, they’ve actually gotten worse.
To help shape a more informed strategy going forward, Mission Roll Call recently conducted a national survey addressing the subject of suicide prevention. Over 2,100 veterans, family members, and caregivers from all 50 states responded. Their responses were as clear as they are sobering. But they also pointed toward solutions grounded in lived experience and capable of producing real impact.
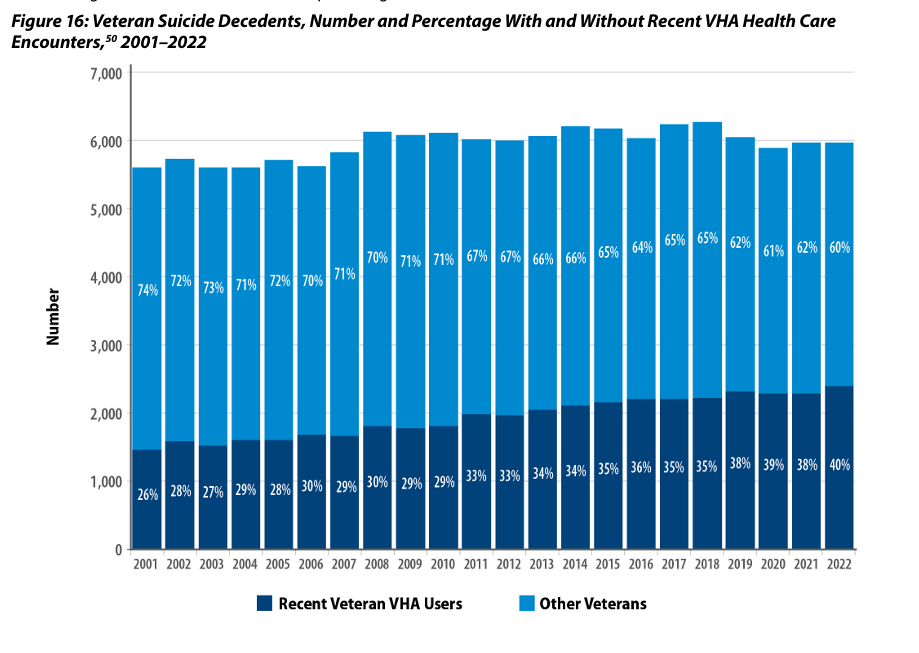
Before we dive into our survey results, it’s important to understand the worsening trend within the staggering numbers of veteran suicides every year. As shown in the chart below from the Department of Veteran Affairs’ 2024 National Veteran Suicide Prevention Annual Report, not only do annual suicide deaths among veterans’ approach or exceed 6,000 per year, but the raw numbers are worsening year over year.
A higher percentage of veterans are dying by suicide
While the number of veteran suicides is increasing, the number of veterans is declining. According to the VA, today there are roughly 18 million veterans, down from over 26 million in 2001. This means a higher percentage of veterans are dying by suicide. And as startling as these facts are, the situation may be even more dire. Owing to various challenges in identifying suicide among veterans, the actual number of veterans dying by suicide is unclear and certainly higher than these figures. As just a few examples, county coroners often struggle to identify the deceased as a veteran and there is no mandatory reporting system for county coroners to report to a central database when they do manage to identify the deceased as a veteran. Also, identifying an overdose death as a suicide remains a challenge unless a note or other demonstration of intent is left behind.
Given this, it makes sense that the VA’s budget allocated to mental health and suicide prevention continues to increase dramatically with each annual budget allocation. That said, these figures, especially when accounting for unknown suicide numbers, demonstrate that current suicide prevention efforts are costing more money and showing worse results.
With that as background, let’s turn to our survey.
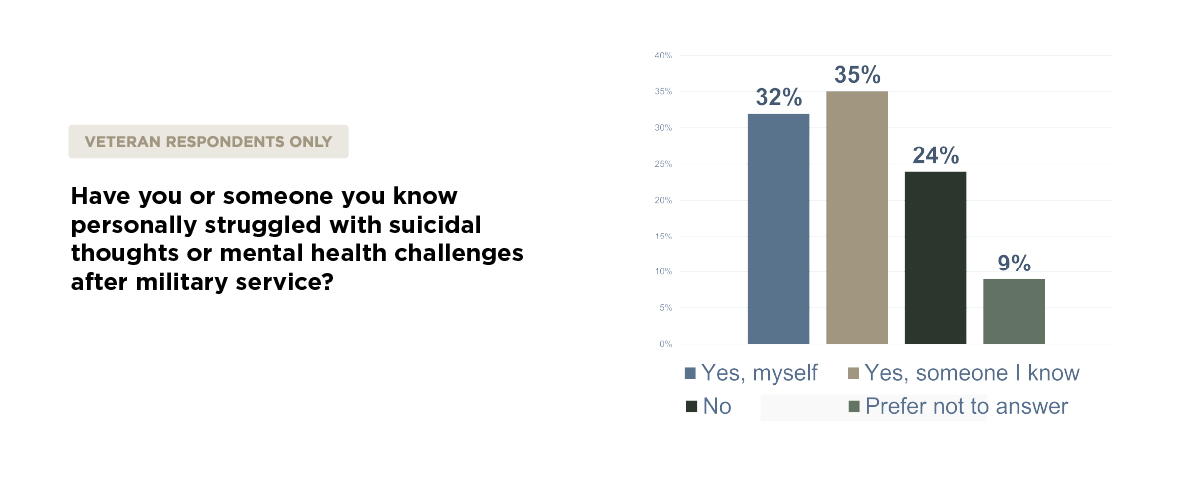
A full two-thirds of veterans struggle with suicidal thoughts
Among only the veteran respondents, a full 67% have either struggled with suicidal thoughts or mental health challenges themselves or know someone personally who has. This figure, extrapolated out over the entirety of the estimated 18 million veterans in the US, means that just shy of 13 million veterans have or might be struggling with mental health challenges or suicidal thoughts.
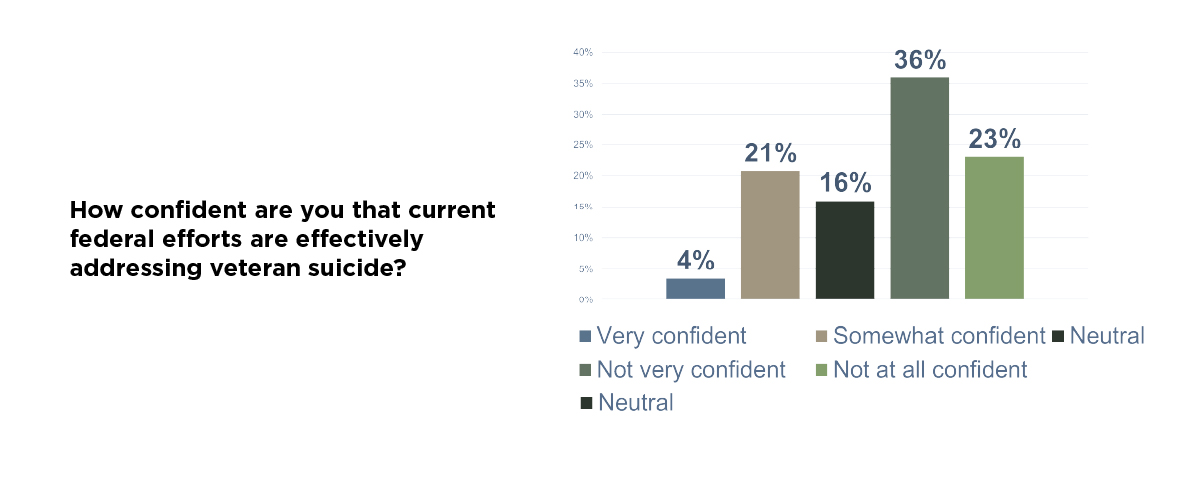
While the total pool of veterans who might benefit from suicide prevention approaches 13 million, at the same time most veterans express little confidence in the federal government’s current approach to preventing suicide.
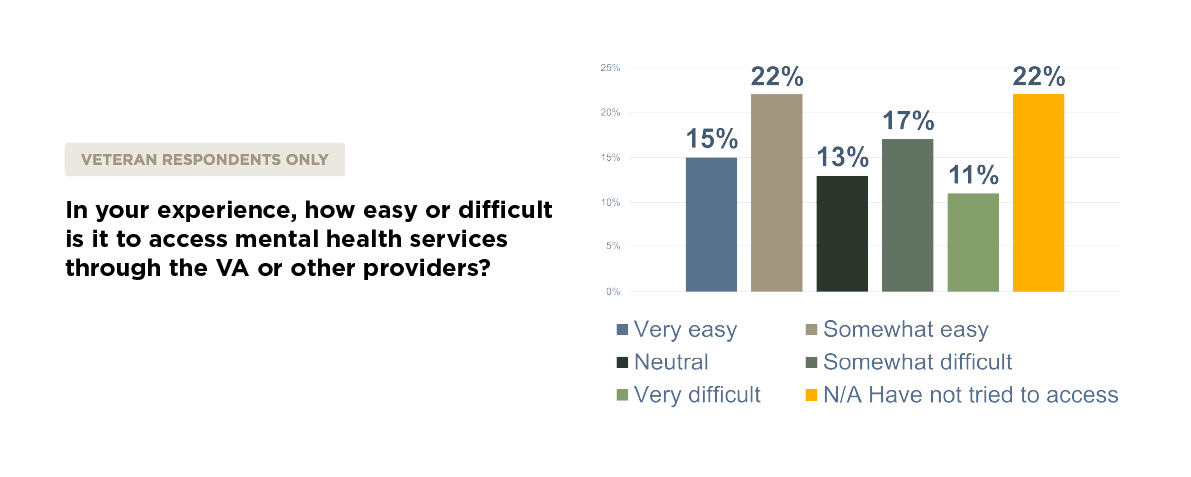
Almost one third of veterans described access to mental health care through the VA or other providers as difficult or very difficult. This aligns with what we’ve heard repeatedly from veterans: the system is often too slow, too bureaucratic, and too disconnected from the day-to-day realities veterans face.
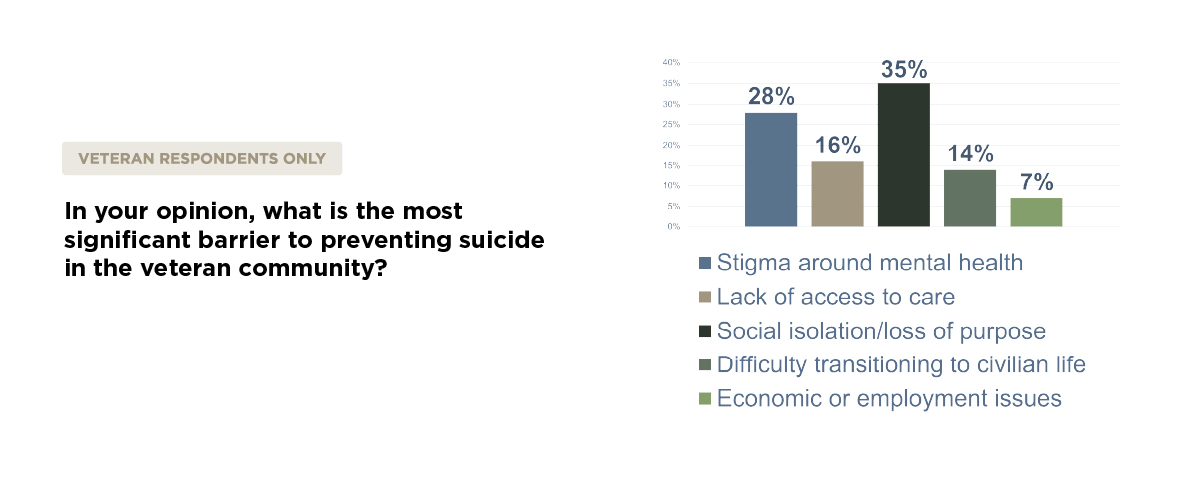
When asked what they see as the biggest barrier to preventing suicide, respondents didn’t point to a lack of funding. They pointed to deeper structural issues—things like stigma around mental health, social isolation, and the struggle to transition into civilian life with a renewed sense of purpose. These are not problems that can be solved by clinical care alone.
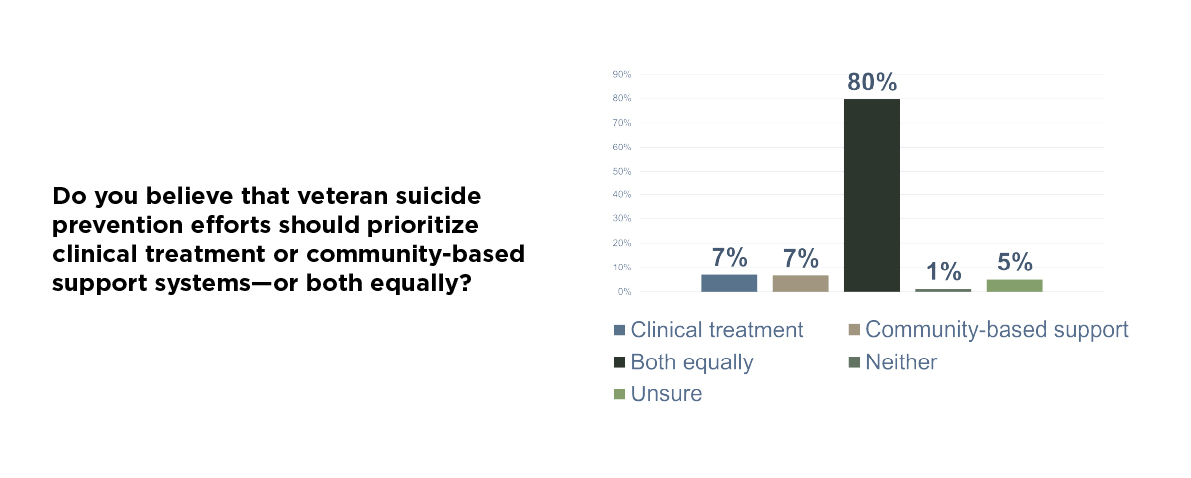
That’s why it’s so important to note what veterans said when we asked them how suicide prevention efforts should be prioritized. A clear majority believe we need both clinical treatment and community-based support, working side by side. This is a strong plea for “all of the above” style solutions and for adhering to the principle of meeting and treating veterans in the manner most meaningful to them.
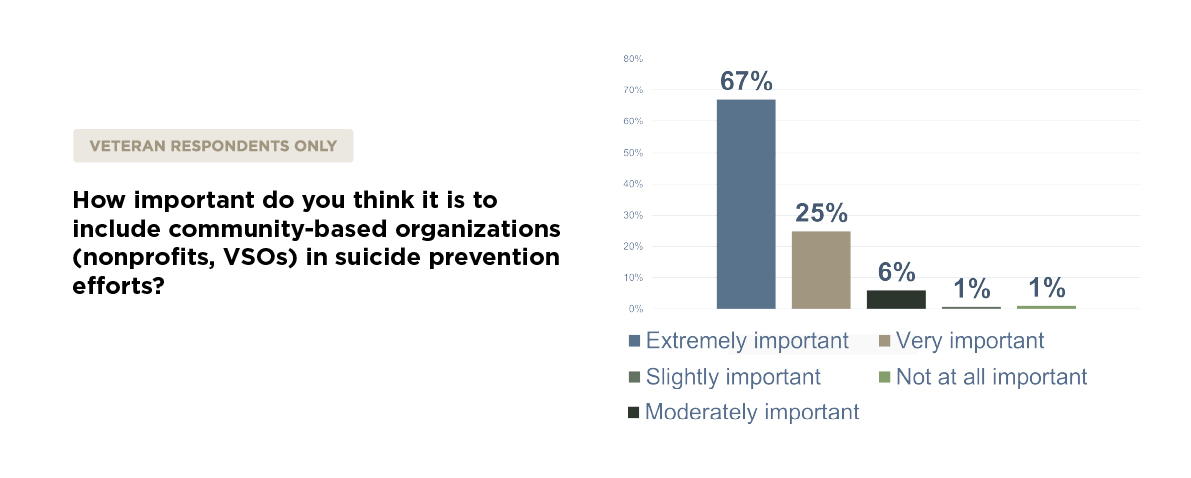
This shouldn’t surprise us. Programs like Team Red, White, and Blue, and The Mission Continues, and other veteran-led initiatives have demonstrated for years that peer connection, physical wellness, and community engagement save lives. And yet, these programs remain underutilized and underfunded.
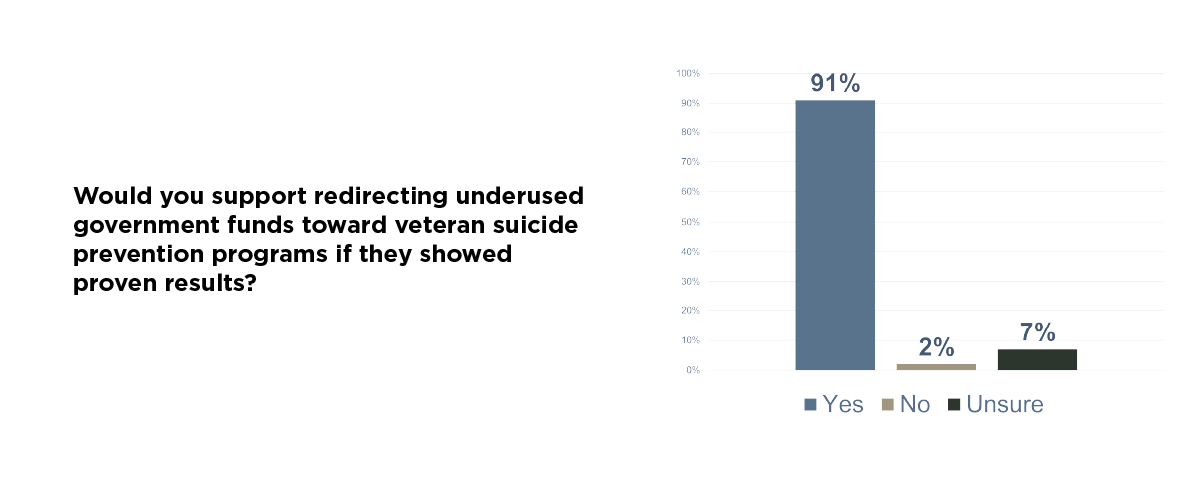
The good news is that veterans overwhelmingly support expanding these types of efforts. They also support creative solutions to pay for them. When we asked about redirecting underused federal funds to support veteran suicide prevention efforts that show proven results, the response was overwhelmingly positive.
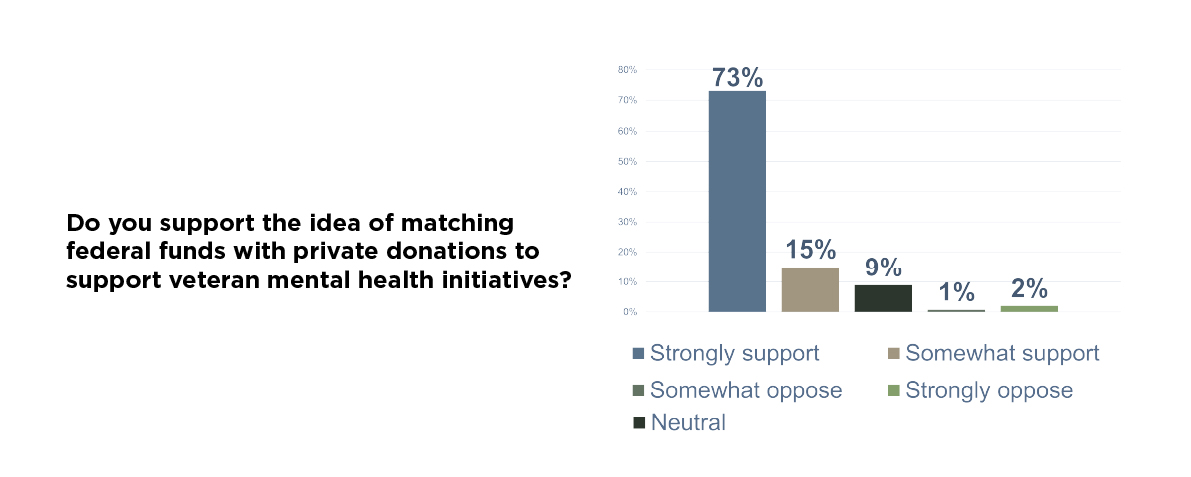
We then asked if veterans would support a federal match for private donations to veteran mental health programs, the answer was again a resounding yes.
These are pragmatic proposals that align with the will of the veteran community and fit within today’s tight fiscal environment. The Fox Grant Program is one example—designed to channel resources into local, community-based solutions. But its implementation has been rocky. Many worthy organizations have struggled to navigate the bureaucracy needed to receive funding. The message we are hearing from veterans is simple: simplify it, expand it, and pair it with a federal match to increase impact.
Another area of near-universal agreement? Training. When asked how important suicide risk identification training is for veterans and their families, the overwhelming majority said it was essential. This is low-cost, high-impact work that can be deployed nationwide with the right partnerships in place.
Giving family members and caregivers the tools to recognize early signs of distress can make all the difference. Veterans are far more likely to confide in a spouse, sibling, or close friend than in a clinician or crisis line. Equipping those closest to them with practical training could lead to earlier intervention, stronger support at home, and a greater chance of recovery before crisis strikes.
Veterans don’t want to rely solely on crisis lines. They want the people around them to be prepared and empowered.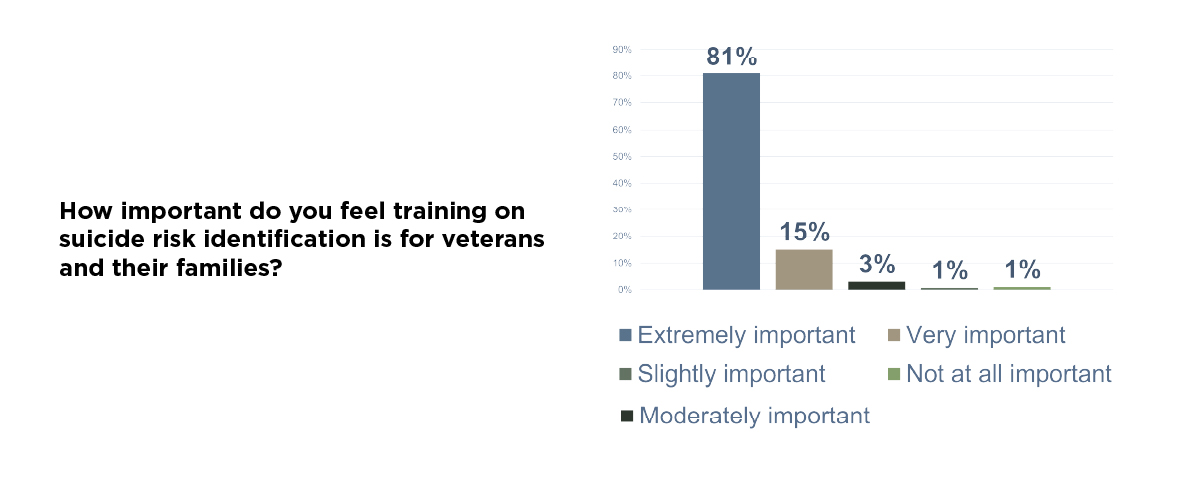
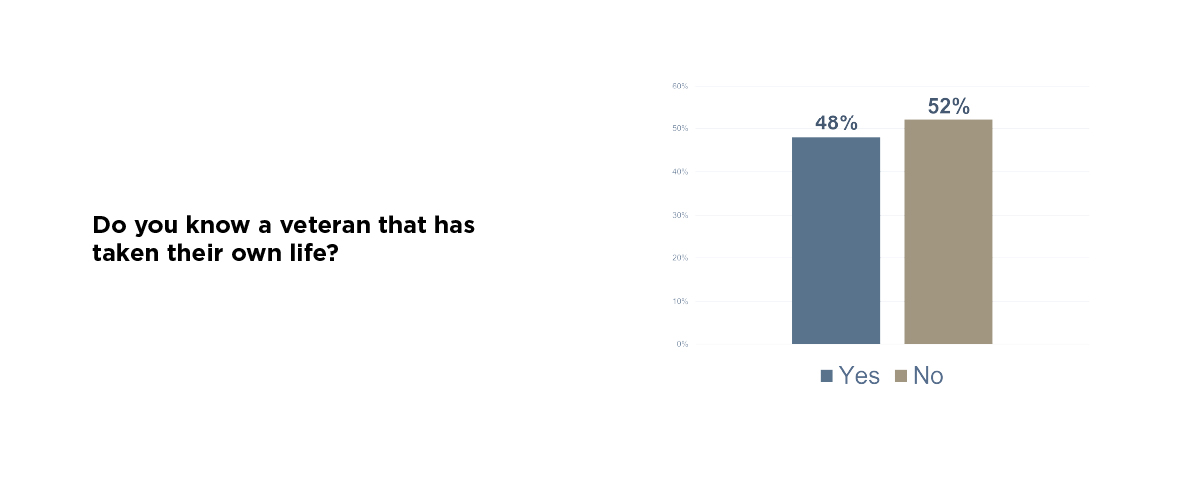
The most personal responses we received weren’t multiple-choice. They were answers to two simple questions: Do you know a veteran who has taken their own life? And as we opened with above, Have you or someone you know struggled with suicidal thoughts or mental health challenges after military service?
The volume of yes answers to both was staggering. These are not distant, abstract issues for most of the veteran community. They are immediate and they are personal. And they are, in many cases, ongoing.
This country has shown that when it decides something matters, we can move fast and think big. We did it with the PACT Act. We’ve done it with housing. We need that same urgency now when it comes to suicide prevention.
Veterans are not asking for more slogans or awareness campaigns. They’re asking for access, purpose, and connection. They want to see the system reoriented toward prevention and away from just managing crisis. They want to be seen not as patients, but as leaders and contributors in building the solution.
We’ve been at this for more than two decades. We’ve spent billions. The numbers haven’t moved. Improving suicide prevention isn’t a funding issue. It’s a strategy, vision, and implementation issue.
It’s time to re-center this fight around what veterans are telling us they need—and what the data increasingly supports. We have models that work. What we need now is focus and follow-through.
Veterans are speaking clearly. The model for addressing veteran suicide isn’t working as it should be. It’s time for Washington to listen.
At Mission Roll Call, we aim to amplify the voices of veterans to create positive, lasting change for the veteran community. We do so based on data informed through surveys of the veteran community.
We launched a nationwide survey on the Veterans ACCESS Act of 2025, a bipartisan piece of legislation that aims to improve access to community-based care and mental health services for veterans. Almost 1,300 respondents weighed in and their message to Congress is clear: where VA healthcare is concerned, veterans want more flexibility, more transparency, and more control over their own care.
We conducted this poll in May 2025 as the ACCESS Act of 2025 is gaining traction in both the House and Senate Veterans’ Affairs Committees. Later this Congressional session, policymakers will be debating how far to go in expanding community care options, often a lightning-rod issue in Washington. Some are concerned about the potential impact on the VA’s infrastructure and its ability to deliver care. Others are pushing for a more veteran-centered model that removes red tape and prioritizes individual choice. We wanted to make sure the people most affected by this legislation had a direct way to weigh in.
Our survey reached 1,292 respondents in all 50 states. Eighty-five percent identified as veterans. The rest were family members, active-duty personnel, national guard, reservists, or civilians who care about the veteran community. The results signal a demand for action and a valuable consideration to inform the political debate in Washington.
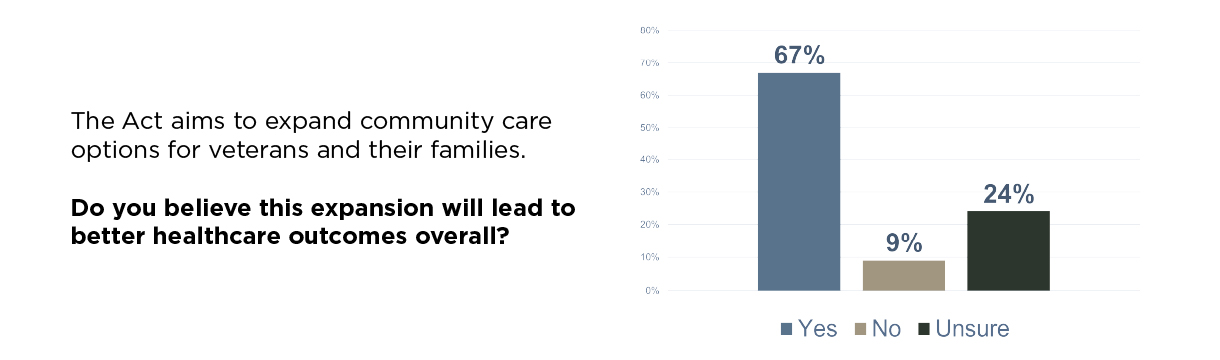
Veterans overwhelmingly support the core provisions of the ACCESS Act.
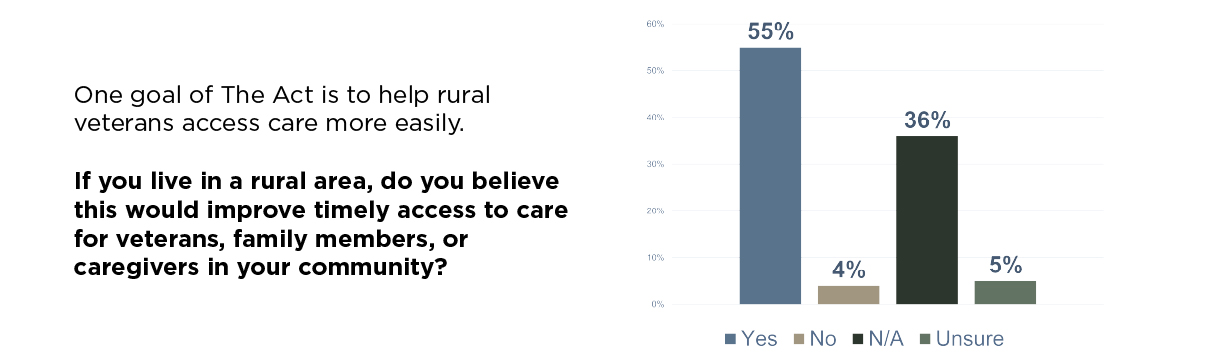
Support for the broader expansion of community care is strong. Sixty-seven percent of respondents believe this legislation will improve healthcare outcomes overall. For rural veterans, the support is even more decisive. Seventy-one percent of those living in rural areas said the ACCESS Act would improve timely access to care in their communities. Too often, distance and travel time create real barriers to care for rural veterans. Giving them the option to receive treatment from a qualified local provider isn’t just a matter of convenience, it can be the difference between getting help and going without it.
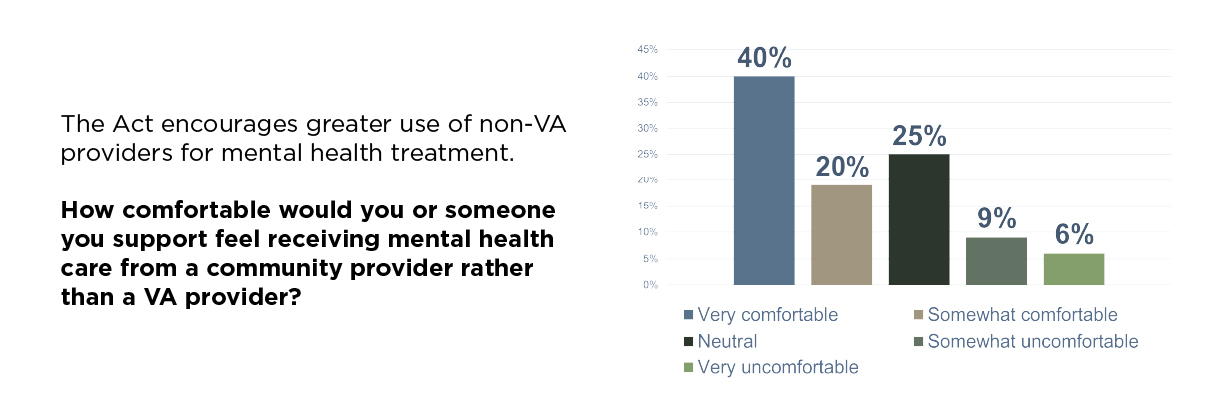
We also asked about comfort with community providers, particularly for mental health services. A full 60% percent of veterans said they were either very comfortable or comfortable receiving mental health treatment from a non-VA provider. That’s important because mental health care is deeply personal. What works for one veteran might not work for another. Community-based options open the door to a wider range of providers, specialties, and approaches. Veterans want the ability to choose what works best for them.
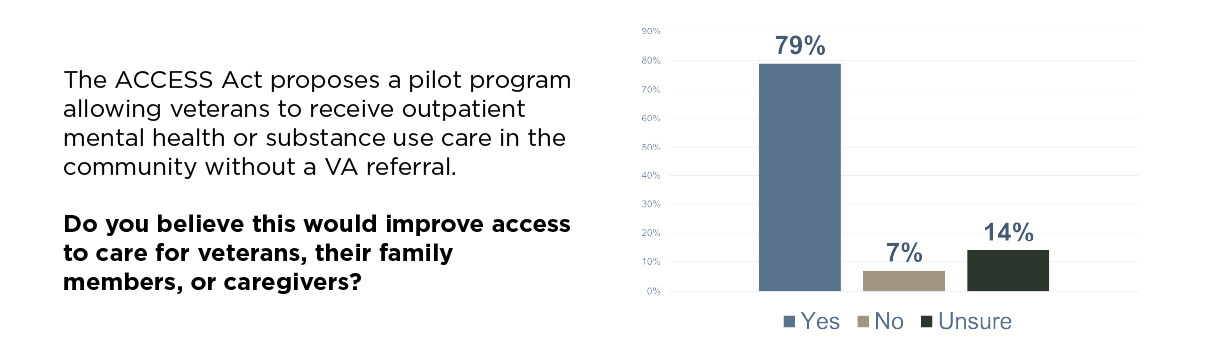
When asked whether allowing veterans, family members, or caregivers to access mental health or substance use care in the community without a VA referral would improve access, 79 percent said yes. This reflects widespread frustration with delays, bureaucracy, and limited access to specialty care within the VA system. Veterans are telling us they don’t want to be forced to wait weeks or months when care is available just down the road.
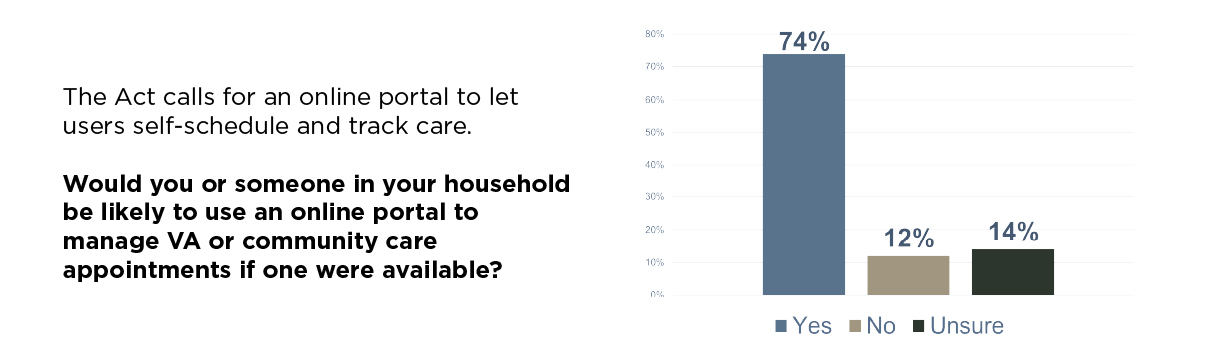
Technology and modernization emerged as high priorities in our polling. Seventy-four percent said they would use an online portal to schedule and track care if one were available. That tells us that veterans are looking for a more user-friendly, efficient way to interact with their healthcare system. They’re used to digital tools in every other part of their lives. They expect the VA to meet them where they are most comfortable.
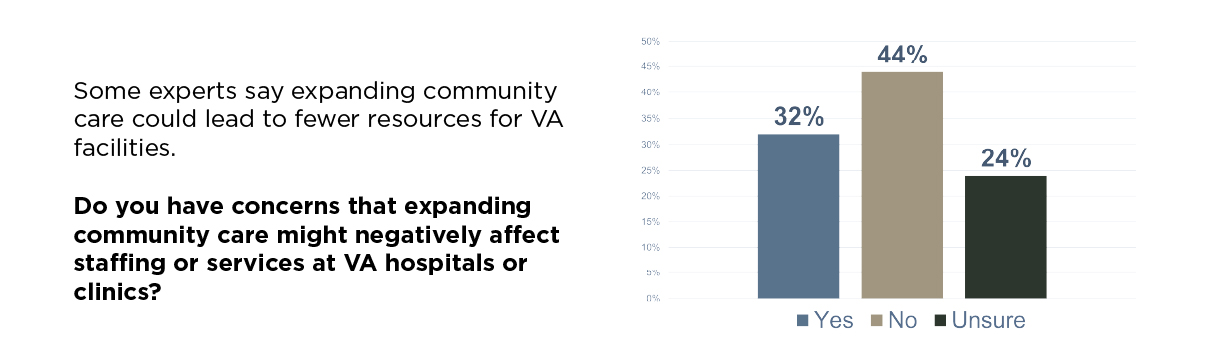
Of course, not all responses reflected full support. Thirty-two percent of respondents expressed concern that expanding community care might reduce staffing or resources at VA hospitals and clinics, with another twenty-four percent being unsure. That concern deserves to be taken seriously. The VA has unique strengths, particularly in specialized areas like prosthetics, polytrauma, and integrated mental health. Our polling suggests that veterans want a strong VA, but they also want choices. Veterans are asking for a system that meets them where they are.
Why This Poll Matters
Too often, decisions in Washington are made based on assumptions about what veterans want. We do our best to replace those assumptions with facts. When Mission Roll Call conducts a poll, we’re creating a direct line between veterans and their elected officials. We’re elevating real voices, not abstract opinions.
That’s especially important in debates like this one, where the stakes are high and the arguments can be emotionally charged. There are valid concerns on both sides. But what often gets lost is the voice of the individual veteran navigating the system, trying to get an appointment, trying to get mental health support, trying to make sense of eligibility rules. Those are the people who should be guiding the conversation. And that’s what our polling allows us to do.
Our approach is rooted in simplicity and clarity. We ask straightforward, non-leading questions. We don’t push a narrative. We ask veterans what they think and then report the results without spin. That gives our advocacy efforts a level of credibility that cuts through the noise. When we walk into a congressional office with more than1,200 responses from across the country, that means something. It’s not just a talking point—it’s a reflection of public will.
How This Shapes Advocacy
We’re already using this data to advocate for the ACCESS Act. We’ve shared our results with members of the House and Senate Veterans’ Affairs Committees. We’ve submitted a Statement for the Record outlining what veterans support and why. We’re working with veteran service organizations, coalition partners, and mental health advocates to make sure this legislation stays focused on what matters most: timely, effective care for those who served.
We’ll continue to keep pressure on. Our advocacy doesn’t end when a bill passes. It extends to how policies are implemented and how they affect veterans on the ground. If a new online portal is promised, we’ll be asking veterans whether it works. If community care networks are expanded, we’ll want to know whether they’re actually accessible and whether veterans are getting the help they need.
This poll was one of our most comprehensive efforts to date, but it won’t be the last. We plan to continue surveying veterans on major legislation, emerging issues, and day-to-day experiences with VA care and more. The more data we collect, the better we can hold the system accountable—and the more effective we can be in Washington.
What Comes Next
Veterans have spoken. They’ve asked for flexibility. They’ve asked for timely access to care. They’ve asked to be treated as informed adults capable of making their own decisions. Congress, the ball is in your court.
To see the full results, click here.
You might know M&M’s for their colorful candy shells and the unforgettable slogan, “melts in your mouth, not in your hand.” But did you know these chocolate treats have military roots?
At Mission Roll Call, we’re always looking for stories that spotlight the ways our military history weaves itself into everyday life. The story of M&M’s is one of innovation, partnership, and a quiet kind of service — bringing comfort to troops when they needed it most.
Born From the Battlefield
In the late 1930s, Forrest Mars Sr.—yes, that Mars—was traveling through Spain during the Spanish Civil War when he noticed soldiers eating small chocolate pellets encased in a hard sugar shell. The candy didn’t melt in their hands or rations, even under the heat of the sun.
Mars took that idea and ran with it. In 1941, he partnered with Bruce Murrie, the son of Hershey Chocolate’s president, to secure a steady chocolate supply. Their collaboration led to the creation of M&M’s, named after the initials of their last names: Mars and Murrie.
Made for War
The original M&M’s weren’t available to the public—they were made specifically for the U.S. military during World War II. The sugar shell meant the chocolate wouldn’t melt in hot or humid conditions, making M&M’s the perfect addition to soldiers’ rations, especially in tropical climates.
They were first packaged in cardboard tubes for easy transport and distribution in the field. And if you needed more proof of their military tie-in, wartime advertisements proudly labeled M&M’s as “100% at War.”
From Rations to Racks
After the war, returning veterans brought their love for M&M’s home. By 1947, the candy was made available to the public. To distinguish their product from imitators, Mars began stamping a small “M” on each candy in 1950—first in black, later changed to the now-familiar white.
The post-war popularity of M&M’s didn’t just reflect good marketing. It reflected something deeper: a shared experience between those who served and the candy that accompanied them through war zones, foxholes, and long deployments.
Still Supporting Service
Decades later, M&M’s continue to support the military community. Mars has partnered with organizations like Operation Gratitude to send care packages filled with M&M’s to deployed troops, offering a taste of home no matter where in the world they’re serving.
M&M’s have even made their way into space, included in NASA’s rations for astronauts. If that doesn’t prove their reliability under pressure, nothing will.
A Reminder of Resilience
M&M’s may not wear a uniform, but their history is rooted in service. They represent ingenuity under pressure, comfort in tough conditions, and the kind of simple joys that can carry us through hard days.
So next time you grab a handful of M&M’s, take a moment to remember their origins and the service members they were created to support. These stories, big and small, are threads in the larger fabric of our military history.
As we celebrate 250 years of military service and sacrifice, Mission Roll Call is committed to preserving that full story—every background, every era, every voice. Be part of the movement to honor these milestones and ensure they’re never forgotten. Join us in the $25 for 250 campaign today.
Mission Roll Call CEO Jim Whaley Meets with VA Secretary Doug Collins for a VSO Breakfast Discussion
Secretary Collins Emphasizes the VA Will Not Cut Veteran Health Services or Benefits.
Mission Roll Call’s CEO Jim Whaley was in Washington, D.C. on March 20th at the invitation of VA Secretary Doug Collins for his first breakfast discussion with Veteran Service Organizations (VSO) since taking the helm at the VA. During this breakfast, Secretary Collins outlined the VA’s plans to implement personnel cuts and reductions. Consistent with his public statements on these cuts, Secretary Collins assured the gathered VSO representatives that veterans would not see any cuts or reductions in their health care or service benefits. 
Secretary Collins also discussed the VA’s focus on improving delivery of care and services to veterans through increased use of community care options. Through our polling and communication efforts with veterans, Mission Roll Call has studied veteran preferences regarding the liberal use of community care. Most veterans support community care as a means to put the veteran at the center of their own care decisions, to ease wait times for care, and to reduce travel and time commitments many veterans face to receive care at VA facilities.
Finally, Secretary Collins shared that much of the work currently being done at the VA involves streamlining many of the byzantine and duplicative administrative systems and processes put in place over the decades. He shared the focused effort to review contracts and seek areas of savings and performance improvements. As one example, the VA has over a dozen payroll programs, that combined makes it challenging for the VA to track and evaluate these programs.
Mission Roll Call wasn’t alone at this meeting and were proud to represent the veteran community along with 9 other Veteran Service Organization’s in attendance. This included leadership from the Wounded Warrior Project, AMVETS, Paralyzed Veterans of America, Vietnam Veterans of America, The American Legion, Boulder Crest, the Blinded Veterans Association, Student Veterans of America, and The Independence Fund. We take pride in our partnerships and productive working relationships with these organizations. Their success is beneficial to veterans everywhere.
Mission Roll Call Conducts Survey of Veterans to Help Lead Discussion on VA Cuts
Here at Mission Roll Call we work hard to amplify veteran voices and ensure those voices are heard during pivotal moments in time. Since the Trump administration took office in January 2025, we have seen a focus on government downsizing, including at the VA. Mission Roll Call designed a survey to help us understand the implications of the proposed changes and how veterans and their loved ones feel about these efforts.
To view this survey and include your voice and thoughts, click here.
Though we are still collating results, one aspect of these cuts has become clear through our discussions and communications with veterans. That is the administration’s efforts could be helped and supported through a robust and well-executed communication plan that leads implementation of cuts and changes. Such a plan would help paint a clear picture of the impending changes and alleviate concerns among veterans and their families that proposed cuts might dig into their health care benefits.
Along with our coalition partners, we plan to share your voice directly with Capitol Hill and the VA to help inform and educate them on what these decisions mean for veterans and their families.
Continued Collaboration with Congress on Legislative Efforts
Also during March, Mission Roll Call continued to leverage veteran input to research, educate, and inform the debate on key pieces of legislation progressing through Congress. Most of these are introduced in the House Veterans Affairs Committee, led by Representative and Chairman Mike Bost of Illinois.
Notable among these pieces of legislation are efforts to broaden community care options, to reauthorize grants to help reduce veteran suicide, to protect veterans’ 2nd amendment rights, to protect veterans’ education benefits, and to eliminate co-pays for veterans.
This legislation, and more, is working through Congress’ process of introduction, discussion, markup, and voting. Mission Roll Call is tracking these bills and providing your voices as it helps educate the community and advance efforts in support of veterans.
The Road Ahead
At Mission Roll Call, we don’t just advocate—we take action. Through our polling and direct engagement with veterans and their families across the country, we bring their unfiltered perspectives straight to policymakers. Testifying in Washington, D.C. was a step forward in ensuring that veterans and their loved ones receive the respect, resources, and opportunities they deserve.
But we can’t do it alone. Real change requires a collective effort. If you believe in this mission, join us at Mission Roll Call. We can challenge harmful stereotypes, push for impactful policy changes, and create a better future for veterans and their families. Your voice matters.
Mission Roll Call had a busy month in February, as did Congress.
Mission Roll Call CEO Jim Whaley Testifies Before Congress
Mission Roll Call’s CEO Jim Whaley was in Washington, D.C., on February 25 to testify before the House Veterans’ Affairs Committee (HVAC). His testimony focused on several pressing issues affecting veterans, all rooted in the real concerns we hear from the veteran community daily.
During this hearing, Jim addressed the following key issues, including, access to healthcare, protecting Veterans’ 2nd Amendment rights, holding the VA accountable in their delivery of services and performance, and safeguarding education benefits for Veterans.
To read Mission Roll Call’s blog on Jim’s testimony, click here.
Mission Roll Call’s Strategic Director of Government Affairs and Advocacy, Mike Desmond, provided a video recap of the testimony and legislation. Watch it here.
Mission Roll Call Teams Up With Call of Duty Endowment to Advocate in Washington
Highlighting a Connection Between Negative Public Perceptions of Veterans and How These Contribute to the Military’s Recruiting and Retention Crisis
Last week, Mission Roll Call took to Washington, D.C., to amplify the voices of veterans and their families and advocate for meaningful policy changes. Our team, including CEO Jim Whaley, joined forces with the Call of Duty Endowment (CODE) President Dan Goldenberg and the Marcus Foundation to present the findings of a joint study conducted by Ipsos. This research shed light on the widespread misperceptions about veterans, emphasizing how these inaccuracies negatively impact recruitment, employment, and overall support for those who have served.
To read more about Mission Roll Call’s blog on our work with Call of Duty Endowment in DC in February, click here.
Mission Roll Call Supports Dr. Paul Lawrence as Deputy Secretary of the VA
On February 19th, the Senate Veterans Affairs Committee (SVAC) held a confirmation hearing for President Trump’s nominee to Deputy Secretary of Veterans Affairs, Dr. Paul Lawrence. You can watch the full hearing here. Mission Roll Call supports Dr. Lawrence’s nomination and signed onto a joint letter of support with other Veteran Service Organizations. The SVAC referred Dr. Lawrence to the full Senate for further hearings and votes, fulfilling the Senate’s Article II constitutional authority to advise and consent the President through approval of certain Presidential nominees.
Mission Roll Call Signs VSO Letter of Support for Senate Budget Language Supporting the Major Richard Star Act
The Major Richard Star Act is an effort within Congress to provide combat-disabled uniformed services retirees with fewer than 20 years of creditable service to concurrently receive, without reduction, veterans’ disability compensation and retired pay or combat-related special compensation.
This legislation was first introduced in 2023, and considered again during Senate budget hearings in January and February for the 119th Congress. Mission Roll Call joined a host of other VSO’s in providing a Letter of Support to SVAC Ranking Member Blumenthal (D-CT), supporting this prudent and impactful legislation.
House Veterans Affairs Committee Holds Robust Slate of Hearings in February
The HVAC had an aggressive hearing schedule in February, holding seven hearings during the month on a range of crucial topics. To go direct to these hearings, click here.
These hearings discussed important issues like improving VA’s Community Care options, VBA Education Benefits, and improving the VA’s Electronic Health Record Modernization effort.
The Road Ahead
At Mission Roll Call, we don’t just advocate—we take action. Through our polling and direct engagement with veterans and their families across the country, we bring their unfiltered perspectives straight to policymakers. Testifying in Washington, D.C. was a step forward in ensuring that veterans and their loved ones receive the respect, resources, and opportunities they deserve.
But we can’t do it alone. Real change requires a collective effort. If you believe in this mission, join us at Mission Roll Call. We can challenge harmful stereotypes, push for impactful policy changes, and create a better future for veterans and their families. Your voice matters.
Last week, Mission Roll Call took to Washington, D.C., to amplify the voices of veterans and their families and advocate for meaningful policy changes. Our team, including CEO Jim Whaley, joined forces with the Call of Duty Endowment (CODE) President Dan Goldenberg and the Marcus Foundation to present the findings of a joint study conducted by Ipsos. This research shed light on the widespread misperceptions about veterans, emphasizing how these inaccuracies negatively impact recruitment, employment, and overall support for those who have served.
Challenging Misperceptions About Veterans
The joint study revealed alarming statistics about the public’s view of veterans:
- More than 80% of Americans believe veterans suffer from severe mental health issues.
- Over 70% think veterans are unemployable and financially unstable.
- More than half believe veterans do not contribute to their communities.
- Two-thirds of Americans think veterans are poorly supported by the federal government.
These misconceptions create significant barriers for veterans transitioning to civilian life and contribute to the ongoing military recruitment crisis. To combat this, Mission Roll Call and CODE are advocating for policy reforms and increased public awareness to reshape how veterans are perceived and supported in America.
Policy Recommendations for Lasting Change
During our meetings with congressional leaders, we outlined four key recommendations to enhance veteran support and change public perception:
- Create a Veteran Wellbeing Accountability Dashboard – A public system that tracks government spending and effectiveness in six key veteran wellbeing areas: employment, mental health, brain health, physical health, housing, and education.
- Redirect Funding to Proven Nonprofits – Shifting government funds toward organizations that have demonstrated measurable success in improving veteran outcomes, ensuring more efficient use of resources.
- Launch a National Veteran Awareness Campaign – A long-term, multi-platform campaign highlighting veterans’ positive contributions and achievements to correct harmful stereotypes.
- Educate High School Staff on Military Careers – Partnering with the Department of Defense and veteran organizations to provide accurate information about military service and post-service opportunities to key influencers like teachers and counselors.
The study reinforced that veterans are among the most engaged and productive members of society. They vote at higher rates, volunteer in their communities, and excel in the workforce. Changing the narrative around veterans isn’t just about recognition—it’s essential to ensuring the future strength of our all-volunteer military force.
The Road Ahead
At Mission Roll Call, we don’t just advocate—we take action. Through our polling and direct engagement with veterans and their families across the country, we bring their unfiltered perspectives straight to policymakers. Testifying in Washington, D.C. was a step forward in ensuring that veterans and their loved ones receive the respect, resources, and opportunities they deserve.
But we can’t do it alone. Real change requires a collective effort. If you believe in this mission, join us at Mission Roll Call. We can challenge harmful stereotypes, push for impactful policy changes, and create a better future for veterans and their families. Your voice matters.
Mission Roll Call’s CEO Jim Whaley was in Washington, D.C., on February 25 to testify before the House Veterans’ Affairs Committee (HVAC). His testimony focused on several pressing issues affecting veterans, all rooted in the real concerns we hear from the veteran community daily.
Mission Roll Call’s Strategic Director of Government Affairs and Advocacy, Mike Desmond, provided a video recap of the testimony and legislation. Watch it here.
Watch the entire hearing here or watch Jim Whaley’s testimony below.
During this hearing, Jim addressed the following key issues:
- Access to Healthcare – While the MISSION Act of 2018 improved some aspects of veteran healthcare, many veterans still struggle with excessive wait times and long travel distances. Mission Roll Call supports the Veterans ACCESS Act of 2025, which prioritizes:
- Enforcing reasonable time and distance standards for care.
- Clarifying wait-time rules to reduce unnecessary delays.
- Expanding veteran choice in healthcare access.
- Ensuring mental health services are prioritized.
- Protecting Second Amendment Rights – Currently, over 270,000 veterans have been added to the FBI’s NICS database simply for using a fiduciary to manage their benefits. The Veterans 2nd Amendment Protection Act ensures due process before a veteran’s constitutional rights can be restricted.
- Holding the VA Accountable – The Restore VA Accountability Act of 2025 aims to enforce higher standards of service within the Department of Veterans Affairs, ensuring that veterans receive the care and benefits they deserve without bureaucratic roadblocks.
- Safeguarding Educational Benefits – The Student Veteran Benefit Restoration Act of 2025 protects veterans from losing their educational benefits due to circumstances beyond their control, ensuring they can complete their education without unnecessary financial hardship.
The Road Ahead
At Mission Roll Call, we don’t just advocate—we take action. Through our polling and direct engagement with veterans and their families across the country, we bring their unfiltered perspectives straight to policymakers. Testifying in Washington, D.C. was a step forward in ensuring that veterans and their loved ones receive the respect, resources, and opportunities they deserve.
But we can’t do it alone. Real change requires a collective effort. If you believe in this mission, join us at Mission Roll Call. We can challenge harmful stereotypes, push for impactful policy changes, and create a better future for veterans and their families. Your voice matters.
Watch Jim’s Testimony
After the historic election in November 2024, the 119th Congress was sworn in and convened on January 3, 2025, and went straight to work on issues directly impacting veterans and their families.
On January 22nd, the full House Veterans Affairs Committee (HVAC) held a hearing addressing community care. Mission Roll Call provided a Statement for the Record, including supporting data from your poll responses, that demonstrates the need for the Department of Veterans Affairs (VA) to improve on delivering care to Veterans through more active use of the community care option. Watch the hearing
In a follow-up to the full HVAC hearing addressing Community Care, the Senate Veterans Affairs Committee (SVAC) convened a separate hearing addressing community care on January 28th. The SVAC heard testimony detailing administrative and bureaucratic shortcomings in the VA’s community care system. Senators discussed some of the causes of these shortcomings, particularly considering the MISSION Act’s express intent to solve many of these problems.
Following these two hearings, HVAC Chairman Mike Bost, and SVAC Chairman Jerry Moran, introduced legislation to increase access to care for veterans through VA providers in the community. Watch the hearing
On January 23, the House subcommittee on Disability Assistance and Memorial Affairs (DAMA) held a hearing on the VA’s practice of reporting Veterans with fiduciaries to the National Instant Criminal Background Check System (NICS) database, restricting their Second Amendment rights. Mission Roll Call joined a pre-hearing roundtable to ensure Veterans’ voices were heard. Watch the hearing
February is already shaping up to be an equally busy month for Advocacy. We will keep you posted as major developments impacting Veterans come up!
Your voice informs our action. Share yours and join our polls.
At Mission Roll Call, we believe that veterans and their families are the most important voices when it comes to shaping policies that affect their lives. No one understands the challenges veterans face better than they do. That’s why we make it our mission to amplify their voices, ensuring they are heard by policymakers, the media, and the public.
Through media appearances, polling, and direct engagement with government leaders, we strive to elevate the insights of those who have served our country. By speaking out, veterans and their families play a crucial role in informing policy and driving the changes that can make a real difference in their communities.
Here are three key advocacy efforts that Mission Roll Call helped champion, all driven by the voices of the veteran community:
1. Veterans 2nd Amendment Protection Act
The Veterans 2nd Amendment Protection Act is a pivotal piece of legislation addressing the rights of veterans. Under the Brady Act of 1993, if the VA appoints a third party to manage a veteran’s compensation, that veteran is automatically referred to the FBI firearms list, restricting their ability to purchase firearms—without due process in court. The VA is the only federal agency that implements this policy without a judicial ruling.
Mission Roll Call took action by surveying our veteran members, and 83% said Congress should change the law to protect veterans’ due process rights. Armed with this data, we met with members of Congress and testified at a House VA Committee Hearing. The outcome? The Veterans 2nd Amendment Protection Act passed the House of Representatives—a victory for veterans’ rights and due process.
2. VA Electronic Health Records Management (EHRM) Poll
The VA’s Electronic Health Records Management (EHRM) system was intended to revolutionize veteran care by creating a seamless transition of medical records from active-duty service to veteran status. However, the system has been plagued by glitches, causing 148 instances of patient harm while operating in only a few VA facilities. With revised cost estimates soaring to $50 billion over 28 years, the question arose: Should the EHRM rollout continue or remain paused until improvements are made?
Mission Roll Call conducted a poll, and 84% of our respondents said the rollout should be paused until the system is improved and certified. We used this data to inform House VA Committee negotiations on HR 2809, advocating for more effective solutions to protect veteran care and taxpayer dollars. Our voice helped shape the ongoing conversation about the future of the EHRM program, ensuring that the focus remains on the well-being of veterans and their families.
3. Changing the VA Motto Poll
The VA’s historic motto, a direct quote from President Lincoln’s second inaugural address, reads: “To care for him who shall have borne the battle and for his widow, and his orphan.” While the motto has honored veterans for decades, critics have pushed for a more inclusive, gender-neutral update, reflecting the growing number of women veterans using VA facilities.
In response, Mission Roll Call surveyed our members, and 70% supported changing the motto to better reflect the diverse veteran community. We provided this data to the VA as they considered the change, and earlier this year, the VA announced its updated motto: “To fulfill President Lincoln’s promise to care for those who have served in our nation’s military and for their families, caregivers, and survivors.” This inclusive change represents the evolution of the veteran community and the VA’s commitment to serving all veterans.
Why Your Voice Matters
The success of these advocacy efforts wouldn’t have been possible without the input of our veteran members and their families. Every poll, every conversation, and every piece of feedback empowers us to fight for the changes that matter most to veterans and their families. Your voice is essential in driving the policies that impact veterans’ lives every day.
Join Mission Roll Call today and make sure your perspective is part of the conversation. With your help, we can continue to enact real, meaningful change—ensuring that veterans receive the respect, care, and rights they deserve. Become a member of Mission Roll Call.